Africa is witnessing an exponential rise in cholera cases amid a global surge. Cases recorded on the continent in the first month of 2023 alone have already risen by more than 30% of the total caseload reached in the whole of 2022.
An estimated 26 000 cases and 660 deaths have been reported as of 29 January 2023 in 10 African countries facing outbreaks since the beginning of the year. In 2022 nearly 80 000 cases and 1863 deaths were recorded from 15 affected countries. If the current fast-rising trend continues, it could surpass the number of cases recorded in 2021, the worst year for cholera in Africa in nearly a decade. Average case fatality ratio is currently almost at 3%, above the 2.3% reached in 2022, and far exceeding the acceptable level of below 1%.
The bulk of the new cases and deaths have been recorded in Malawi, which is facing its worst cholera outbreak in two decades. Malawi’s neighbours Mozambique and Zambia have also recently reported cases. In East Africa, Ethiopia, Kenya and Somalia are responding to outbreaks amid a prolonged and harsh drought that has left millions of people in dire need of humanitarian assistance. Burundi, Cameroon, Democratic Republic of the Congo and Nigeria have also reported cases.
“We are witnessing a worrying scenario where conflict and extreme climatic events are worsening the triggers of cholera and increasing its toll on lives,” said Dr Matshidiso Moeti, World Health Organization (WHO) Regional Director for Africa. “It’s critical for African countries to scale up readiness to quickly detect cases and mount a comprehensive and timely response. We are supporting governments to bolster key control measures to halt these outbreaks as quickly as possible.”
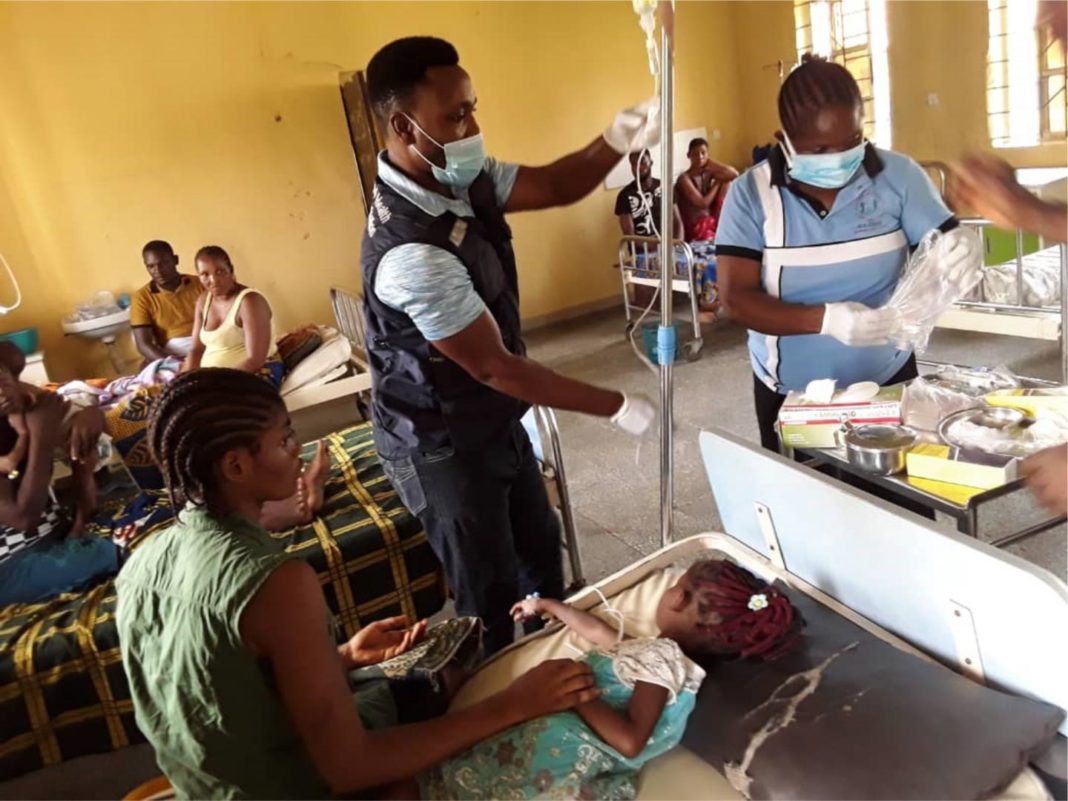
WHO is working with countries to ramp up disease surveillance, prevention and treatment measures, community engagement, as well as multi-sectoral coordination with partners and agencies to improve sanitation and provide safe water. The Organization has deployed 65 experts to five African countries, including 40 to Malawi. In addition, WHO has also disbursed US$ 6 million to kick-start emergency cholera response in Kenya, Malawi and Mozambique.
So far this year, around 3.3 million cholera vaccine doses have been delivered to the Democratic Republic of the Congo, Kenya and Mozambique—which is to take delivery in the coming days—through the International Coordinating Group on Vaccine Provision. This initiative aims to manage emergency supplies of vaccines and is a partnership of the International Federation of the Red Cross and Red Crescent Societies, Médecins sans Frontières United Nations Children’s Fund and WHO.
The increase in cholera outbreaks globally has put a huge strain on the availability of vaccines, prompting the International Coordinating Group on Vaccine Provision to temporarily suspend the standard two-dose vaccination regimen in cholera outbreak response campaigns, using instead a single-dose approach. A further surge in cholera outbreaks risks deepening the shortage.
Cholera is an acute, extremely virulent infection that can spread rapidly and dehydration results in high morbidity and mortality. However, the disease is easily treatable. Most people can be treated successfully through prompt administration of oral rehydration solution or intravenous fluids.
“Every death due to cholera is preventable,” said Dr Moeti. “This disease is much a health challenge as it is a development one. As such investments in better sanitation and access to safe water formidably complement the public health initiatives to sustainably control and end cholera.”
Effective control relies on implementing comprehensive measures including enhanced epidemiological and laboratory surveillance to detect, confirm and quickly respond to outbreaks, improving access to treatment, vaccines, safe water and basic sanitation as well as effecting behavioural change and better hygiene practices among communities.
The cholera outbreaks in Africa are occurring in the context of extreme climatic events, conflicts, ongoing outbreaks of other disease such as wild poliovirus as well as limited financial resources and strained health workforce due to the response to the COVID-19 pandemic.